Impaired Physical Mobility NCP Rheumatoid Arthritis
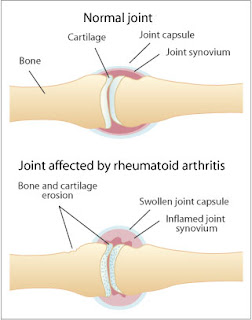
Rheumatoid arthritis is an inflammatory arthritis and an autoimmune disease. This is where the body’s immune system attacks healthy tissues in the body, particularly the synovium the membrane joining the joints. The joints fill with fluid, due to this process and cause pain and systematic inflammation.
Rheumatoid arthritis is not only a condition linked with joints. It causes innumerable problems in other organs also such as eyes, lungs, skin and heart. Almost all of these problems are uncommon nevertheless they are crucial too, when they make their presence. Basically rheumatoid arthritis comes under the group of autoimmune diseases and hence it can make its presence in any part of the body once it catches hold of joints.
Rheumatoid arthritis is a chronic disease that may have periods of intense activity followed by a period of inactivity. Some patients may go through continuous activity that becomes worse with time. Organ damage and disability can occur with continuous rheumatoid arthritis.
The symptoms of rheumatoid arthritis come and go, depending on the degree of tissue inflammation. When body tissues are inflamed, the disease is active. When tissue inflammation subsides, the disease is inactive (in remission).
When the disease is active, symptoms can include fatigue, loss of energy, lack of appetite, low-grade fever, muscle and joint aches, and stiffness. Muscle and joint stiffness are usually most notable in the morning and after periods of inactivity.
Nursing Diagnosis: Impaired Physical Mobility
Related to:
- Skeletal deformity
- Painful
- Discomfort
- Activity intolerance
- Decreased muscle strength.
- Reluctance to try moving / inability to move in with their own physical environment.
- Limiting the range of motion, coordination imbalances, decreased muscle strength / control and mass (advanced stage).
- Maintaining a function of position in the absence / restrictions contractures.
- Maintain or improve strength and function of and / or compensation of the body.
- Demonstrate techniques / behaviors enabling activities
1. Evaluation / continue monitoring the level of inflammation / pain in the joints
Rationale: The level of activity / exercise depends on the development / resolution of the inflammatory process.
2. Keep the rest - bed rest / activity schedule sit down if necessary to provide a continuous period and nighttime sleep uninterrupted.
Rationale: Systemic Rest is recommended during acute exacerbations, and all phases of the disease is important to prevent exhaustion maintain strength
3. Assist with range of motion active / passive, and resistive exercise also demikiqan isometris if possible
Rationale: Maintain / improve joint function, muscle strength and general stamina.
4. Change positions frequently with sufficient amount of personnel. Demonstrate / removal of technical aids and mobility aid use, eg, trapeze
Rationale: Eliminates stress on the network and improves circulation. Facilitate patient self-care and independence. Proper removal techniques to prevent tearing skin abrasion.
5. Position with pillows, sandbags, rolls trokanter, splint, brace
Rationale: Increase stability (reducing the risk of injury) and maintain the necessary joint position and body alignment, reducing contractor.
6. Use a small pillow / thin below the neck.
Rationale: Preventing neck flexion.
7. Encourage the patient to maintain an upright posture and sitting height, standing, and walking.
Rationale: To maximize joint function and maintain mobility
8. Provide a safe environment, such as raising the chair, using the toilet railings, wheelchair use.
Rationale: Avoiding injury due to accidents / falls
9. Collaboration: consul with physiotherapy.
Rationale: Useful in formulating training programs / activities based on individual needs and identifying tools.
10. Collaboration: Provide foam mat / converter pressure.
Rationale: Reducing the pressure on the fragile tissue to reduce the risk of immobility.
1 komentar:
If you are diagnosed with RA your primary concern is going to be your joints. But RA is a systemic disease, meaning the inflammation that’s affecting your joints can also target other parts of the body. Living with rheumatoid arthritis? You may qualify for this clinical research study