Nursing Plan for Pneumonia with Diagnosis and Interventions
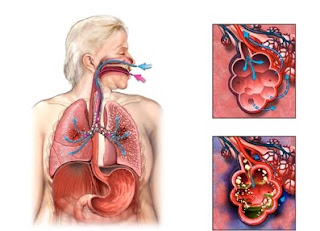
Pneumonia is an infection of the lungs. The lungs are made up of small sacs called alveoli, which fill with air when a healthy person breathes. When an individual has pneumonia, the alveoli are filled with pus and fluid, which makes breathing painful and limits oxygen intake. Many different germs can cause pneumonia, including bacteria, viruses, and fungi.
Causes of Pneumonia
The most common are caused by viruses, including adenoviruses, rhinovirus, influenza virus (flu), respiratory syncytial virus (RSV), and parainfluenza virus (which causes croup).
Symptoms of Pneumonia
The symptoms of pneumonia include:
- rapid or difficult breathing
- cough
- fever
- chills
- loss of appetite
- wheezing (more common in viral infections).
- nasal congestion
- breathing with grunting or wheezing sounds
- vomiting
- chest pain
- abdominal pain
- decreased activity
- nausea
- diarrhea
Some of these tests may include:
- sputum tests (lab tests done on the mucus or phlegm that you cough up from your lungs)
- blood tests
- chest X-rays
Pneumonia can be treated with antibiotics. These are usually prescribed at a health centre or hospital, but the vast majority of cases of childhood pneumonia can be administered managed effectively within the home. Hospitalization is recommended in infants aged two months and younger, and also in very severe cases.
Nursing Plan for Pneumonia
3 Nursing Diagnosis and Interventions for Pneumonia
1. Ineffective airway clearance related to inflammation, secret buildup.
Goal: Effective airway, pulmonary ventilation is adequate and there is no secret buildup.
Nursing Interventions:
- Monitor respiratory status every 2 hours, assess the increase in respiratory status and abnormal breath sounds.
- Perform percussion, vibration and postural drainage every 4-6 hours.
- Give oxygen therapy according to the program.
- Help patients cough up secretions / suctioning.
- Give a comfortable position that allows the patient to breathe.
- Create a comfortable environment so that patients can sleep.
- Monitor blood gas analysis to assess respiratory status.
- Give drink enough.
- Provide sputum for culture / sensitivity test.
- Collaboration of antibiotics and other drugs according to the program.
2. Impaired gas exchange related to changes in alveolar capillary membrane.
Goal: Patients showed improved ventilation, optimal gas exchange and tissue oxygenation adequately.
Nursing Interventions:
- Observation of level of consciousness, respiratory status, cyanosis signs every 2 hours.
- Give Fowler position / semi-Fowler.
- Give oxygen according to the program.
- Monitor blood gas analysis.
- Create an environment that is quiet and patient comfort.
- Prevent the occurrence of fatigue in patients.
3. Fluid Volume Deficit related to inadequate oral intake, fever, tachypnoea.
Goal: Patient will maintain normal body fluids.
Nursing Interventions:
- Record intake and output of fluids. Encourage the mother to continue giving fluids orally and avoid the condensed milk / drink cold or cough inducing.
- Monitor fluid balance in the mucous membranes, skin turgor, rapid pulse, decreased consciousness, vital signs.
- Keep drip infusion accuracy according to the program.
- Perform oral hygiene.
ads
3 komentar:
This blog site is pretty good! How was it made . I view something genuinely interesting about your site so I saved to my bookmarks . You can visit my site.
Respiratory Syncytial Virus treatment
Interesting blog. This is one of my favorite blog also I want you to update more post like this. Thanks for sharing this article.
Home Nurse in Chennai